 4) Atypical RBBB may represent underlying delay in left ventricular (LV) activation as well. The definition may also be applied to a pattern with RBBB criteria in the precordial leads and LBBB criteria in the limb leads, and vice versa ( Fig. 3) Interventricular conduction delay (IVCD) which characterized by wide QRS morphology that does not resemble either typical LBBB or RBBB. 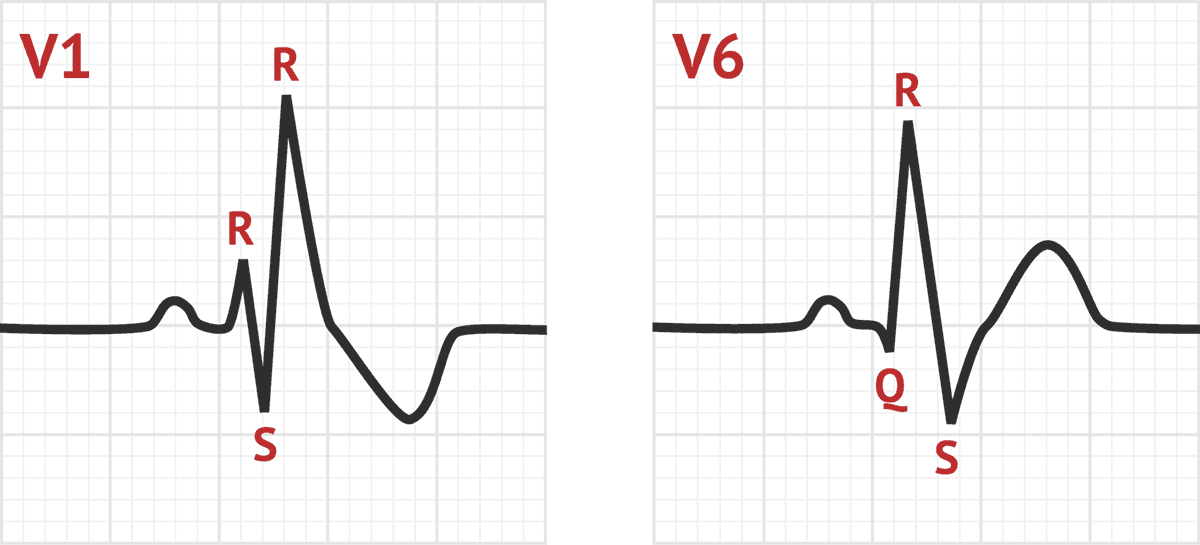
2) Complete (typical) right bundle branch block (RBBB) is described as QRS duration ≥ 120 ms in adults, rsr′, rsR′, or rSR′ in leads V1 or V2, R or r deflection is usually wider than the initial R wave patients, S wave of greater duration than R wave or greater than 40 ms in leads I and V6 in adults, and normal R peak time in leads V5 and V6 but > 50 ms in lead V ( Fig. Non-LBBB wide QRS complex patterns include the following four groups are represented in Figure 1 as follow: 1) Atypical LBBB represent “QRS duration greater than or equal to 120 ms in adults, broad notched or slurred R wave in leads I, aVL, V5, and V6, and an occasional RS pattern in V5 and V6 attributed to displaced transition of QRS complex, absent q waves in leads I, V5, and V6, and R peak time greater than 60 ms in leads V5 and V6” with atypical feature such as Q wave in I and aVL, larger R wave in V1 and V2, or V6 QRS complex morphology which is different from those in I and aVL ( Fig. 
The Non-LBBB Wide QRS Complex Electrocardiogram (ECG) Criteria Furthermore, we conferred the current guidelines, including the comprehensive update of the Canadian Cardiovascular Society (CCS) guidelines for the management of heart failure (HF) 2017, the European Society of Cardiology (ESC) Heart Failure Association guidelines for the diagnosis and treatment of acute and chronic HF 2016, the National Institute of Health and Care Excellence (NICE) guidelines for ICD (implantable cardioverter defibrillator) and CRT for arrhythmia and heart failure 2014, the American College of Cardiology Foundation/American Heart Association guideline for the management of heart failure 2013, the ESC European Heart Rhythm Association guidelines on cardiac pacing and cardiac resynchronisation therapy 2013, and the update to National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand guidelines for the prevention, detection and management of chronic HF in Australia 2011. In this article, we reviewed the major trials that enriched the most recent international guidelines for CRT implantation focusing on the available data about the outcome of using CRT in non-LBBB cohort. It remains uncertain whether patients with non-LBBB QRS complex morphology clearly benefit from CRT or only modestly respond. An important and consistent finding in published systematic reviews and in subgroup analyses is that the benefits of CRTs are maximum for patients with a broader QRS durations, typically described as QRS duration > 150 ms, and for patients with a typical left bundle branch block (LBBB) QRS morphology. However, these alerts often have a high false-positive rate, due to the artifacts mentioned above.Cardiac resynchronization therapy (CRT) benefits have been firmly established in patients with heart failure and reduced left ventricular ejection fraction (HFrEF), who remain in New York Heart Association (NYHA) functional classes II and III despite optimal medical therapy, and have a wide QRS complex. For example, VTach, VFib, Asystole, and AFib are commonly detected by telemetry equipment and reported to personnel in the form of audible and visual alerts. Real telemetry monitoring systems do include more advanced features not seen here, such as dynamic warning of dangerous rhythms. This also wreaks havoc on the automated rhythm warnings generated by telemetry systems! Many factors such as electrode placement, body weight, movement, muscle tremors, shivering, or even pacemakers can cause the EKG signal to become noisy or difficult to read. I have attempted to pick cleaner samples for this site in general, but real patients cause a lot of what we call "artifacts" on EKG monitors. Additionally, the "baseline" of the EKG (which should be at 0 voltage or the exact center of the chart) can also change or vary depending on conditions. You can see just how much amplitude changes from patient to patient simply by looking at samples here. This sometimes requires "zooming in" in order to better see important details. 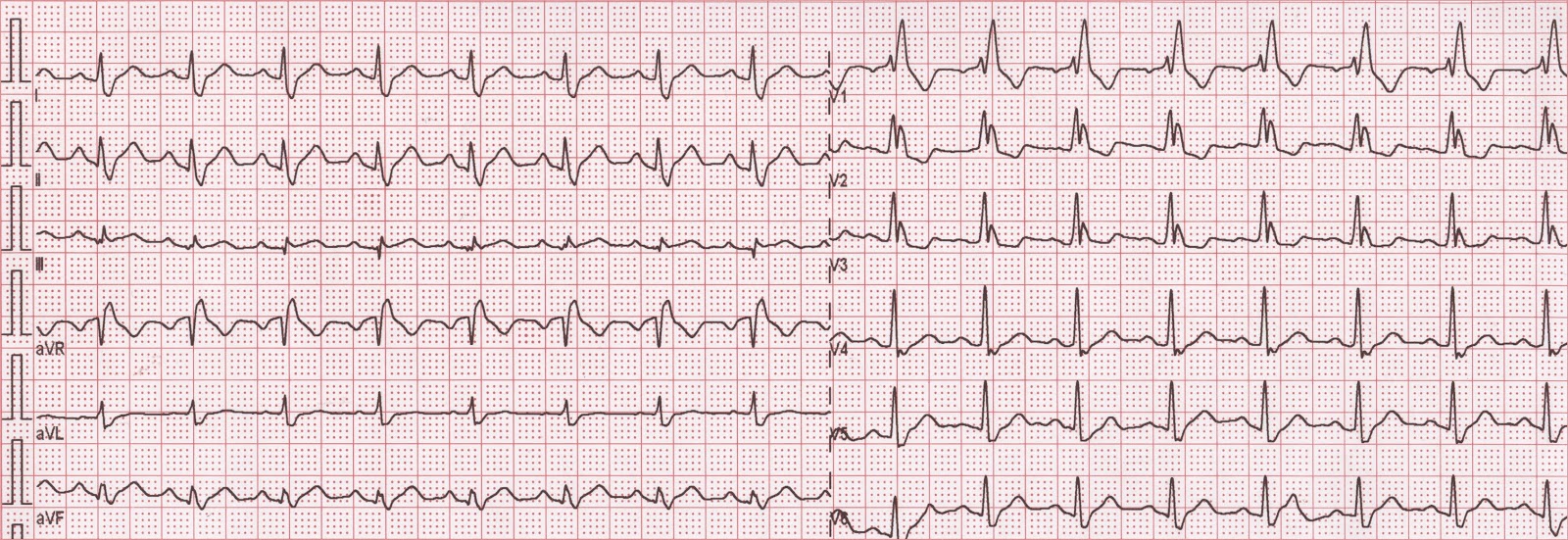
Depending on the patient, electrode placement, and other factors, the amplitude (or height) of the waves can change dramatically. Real telemetry monitors also allow you to adjust the speed and amplitude of the EKG waves. This unique format allows for easy analysis of cardiac rhythms. Telemetry monitors have a unique plotting style, "drawing" the EKG wave across the screen, then overwriting the wave on the next pass. The experience between watching EKGmon and a hospital telemetry monitor is very similar. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
